Postpartum Depression
Female psychiatrist specializing in postpartum depression offers immediate help, including postpartum depression medication and treatment. Contact +1(833)312-4222 for assistance.


What is Postpartum Depression ?
Postpartum depression or postnatal depression is the onset of depressed mood and associated symptoms within the first year of giving birth that is persistent and lasts more than two weeks with or without treatment. It is important to get treatment for postpartum depression because failure to do so can cause long-term adverse effects to both mother and baby.
What are the causes of Postpartum depression ?
- Hormone shifts after giving birth
- Difficult pregnancy
- Anemia
- Sheenhan’s syndrome (Ischemia pituitary gland during delivery)
- Nutritional deficiency
- Genetic
- Previous history of Depression
- Marital / relationship discord
- Chronic fatigue
- Excessive Multitasking


What are the symptoms of Postpartum depression ?
Symptoms of postpartum depression include depressed mood, irritability, fatigue, moodswings, inpatients, feeling numb, feeling disconnected from baby, older children or partner, loss of desire to care for or nurture the baby, feelings of guilt or anger, inability to perform at work, and loss of interest in usual activities.
Postpartum depression can be extremely isolating for mothers, as it occurs at a time in ones life when society expects a mother to feel overjoyed at the arrival of the new baby, and overcome with motherly love. The very nature of postpartum depression, is that a mother is sometimes unable to feel any type of joy and then feels guilty because they are not experiencing the joy in motherhood that they think they ought to feel.
Sometimes mothers are just about able to cope with loving and caring for the baby but do now have the ‘bandwidth.’ for more, such as work, partners, or older children.
How can lack of postpartum depression treatment impact your child ?
Although most mothers suffering from postpartum depression are able to feed their child and provide essential needs to preserve life , other aspects of parenting such as cuddling , kissing, playing , engaging tend to slide. Even a very fun baby may sense a mother’s anxiety irritability and impatience and experience a form of infantile depression caused by anxiety and lack of nurture. Studies have shown that babies and infants with depressed parents suffer from increased risk of anxiety. depression, cognitive impairment, failure to thrive, delayed milestones, delayed speech and failure to form attachments. These babies and infants also suffer increased anxiety and depression as well as difficulties with adult relationships in latter life.
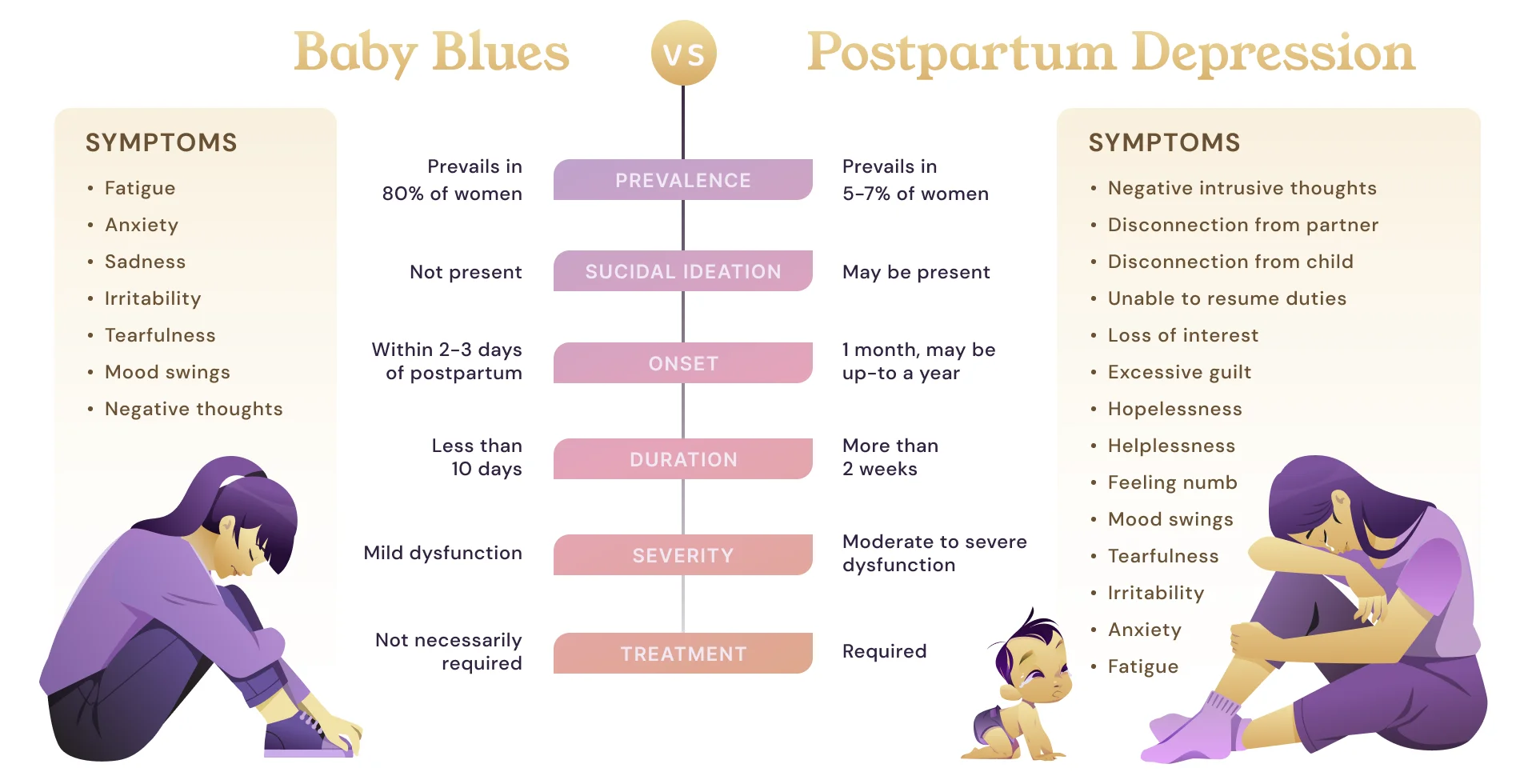
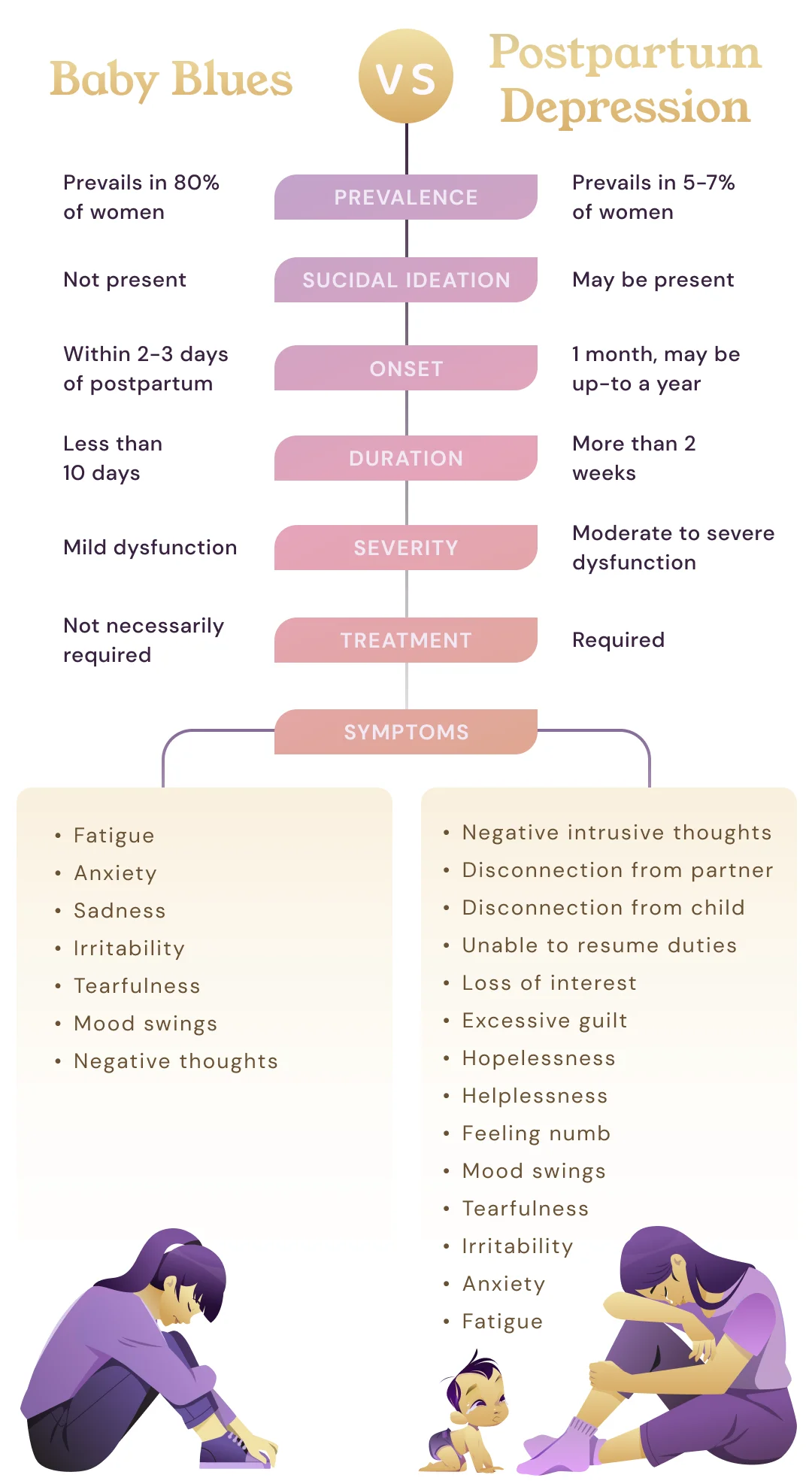
What is the difference between Postpartum depression and the ‘Baby Blues’?
‘Baby Blues,’ is a common condition in around 80 percent of new mothers. It is a period of low mood, anxiety, and irritability that onsets within the first week of giving birth. ‘Baby blues are caused by hormone shifts, especially drops in levels of estrogen, progesterone, and growth hormone after giving birth. It can also be exacerbated by traumatic delivery, sleep deprivation, and fatigue. Baby blues is usually self-limiting and should resolve within two weeks. If symptoms do not resolve within a fortnight, it is important to consider the possibility of postpartum depression and seek advice.
Do I have Postpartum depression ?
Sometimes symptoms of postpartum depression can be atypical and not look like typical major depressive disorder. You may have postpartum depression if you are:
- Feeling low, tearful, or sad
- Feeling irritable
- Feeling disconnected from your baby or other children
- Wanting to hide
- Feeling overwhelmed
- Fighting more with your partner
- Lost interest in intimacy and daily activates
- Feeling numb
- Feeling hopeless about the future
- Having severe mood swings and fluctuations in mood throughout the day
- Feeling hopeless, helpless
- Unable to keep up with chores
- Feeling excessive guilt or believing that you are a bad mother
- Problems with attention and concentration, inability to perform at work
A person with post-partum depression can have normal sleep and appetite and may not meet the DMS criteria for major depressive disorder.
Postpartum Depression Psychiatrist

Dr. Valeria Serban
Postpartum Depression Specialist
Dr Valeria Serban is an experienced neuropsychiatrist. She is passionate about helping young mothers overcome psychiatric symptoms during the pregnancy and postpartum period.
Dr. Serban uses a combination of medication and therapy to help patients through the Postpartum period. Her goal is to help allieviate symptoms, of depression, anxiety, insomnia, panic attacks and help mothers regain control of their lives.
Dr. Serban understands that navigating relationships, career and motherhood is not easy. As well as prescribing medication she also uses psychotherapy and lifestyle management to ensure that new mothers get the support they need during the postpartum period.
Medical School
Neurology Residency Training
Master of Philosophy (M.Ph.) - Neuroscience
Internal Medicine Residency
Neurology Residency
Doctor of Philosophy (Ph.D.) - Neuroscience
Clinical Neurophysiology Fellowship
Board Certification

Dr. Tony Issac
Board Certified Psychiatrist in New York & New Jersey (MD)
Dr. Tony Isaac is a double-board-certified Psychiatrist with nine years of psychiatry experience. He provides compassionate and discreet psychiatric evaluations, including postpartum depression screening and treatment that includes postpartum psychotherapy and sensitive medication titration.
Apart from treating a wide range of psychiatric conditions, which include insomnia, panic attacks, depression, anxiety, OCD, bipolar disorder, and schizophrenia, Dr. Tony Issac is also a postpartum depression specialist who works closely with mothers suffering from addiction, and postpartum depression to achieve a collaborative treatment plan and work towards recovery and healing.
Postpartum depression has an adverse effect on a mother’s ability to bond with her child. Dr. Issac provides high-quality and consistent care to those suffering from postpartum depression and utilizes his expertise to improve symptoms as well as social and occupational functioning.
Dr. Issac also conducts suicide assessments, and acute stabilization and works with the family and employer to provide the required support.
Please schedule online or call +1 (833) 312-4222 to schedule an appointment with Dr. Tony Issac.

Dr. Gundu Reddy
Postpartum Depression Specialist
Dr. Gundu Reddy, a board-certified urgent psychiatrist with fifteen years of experience in clinical psychiatry and ten years of experience in forensic psychiatry, is also an expert postpartum depression psychiatrist. She has trained in Medication Management, psychodynamic psychotherapy, and cognitive behavioral therapy and is interested in integrative psychiatry.
Postpartum depression or maternal depression is linked to grave morbidity for the mother, and must not be left untreated. Timely intervention from an expert postpartum depression psychiatrist is extremely critical.
According to Dr. Reddy, the decision to take postpartum depression medication must be taken seriously and must be prescribed with utmost care. She believes that the goal of medication management, which includes postpartum depression medication management, is to achieve maximum efficacy with minimum side effects and gentle titration.
Please schedule online or call +1(833)312-4222 to schedule an appointment with Dr. Reddy.
Schedule an Appointment with one of our Online Psychiatrists.
Clinical Services: California, Florida, Illinois, New Jersey, New York, South Carolina, Tennessee
Forensic Psychiatry Services: All of the US and Canada
How much does it cost to see an online psychiatrist at Gaba Telepsychiatry?
Your first online appointment with one of our psychiatrists will cost $400. The follow-up appointments will be $250. If you have out-of-network benefits, we can submit claims on your behalf.
What is it like to have Postpartum Depression ?
Postpartum depression can feel just like major depressive disorder. The difference is that the mother has the additional obligation of taking care of a baby, as well as herself and sometimes older children. Sleep deprivation, excessive fatigue, and multiple obligations can get in the way of recovery healing. Mothers who experience postpartum depression can experience extreme guilt, as they may not feel the desire to nurture the newborn. The very nature of depression can cause guilt, and negative intrusive thoughts about oneself. Feeling detached from the newborn or baby, at a time when society and family expect the new mother to feel overjoyed and overcome with love, can feed into the depressive belief by the mother experiencing postpartum depression that they are not a good mother or somehow a bad person.
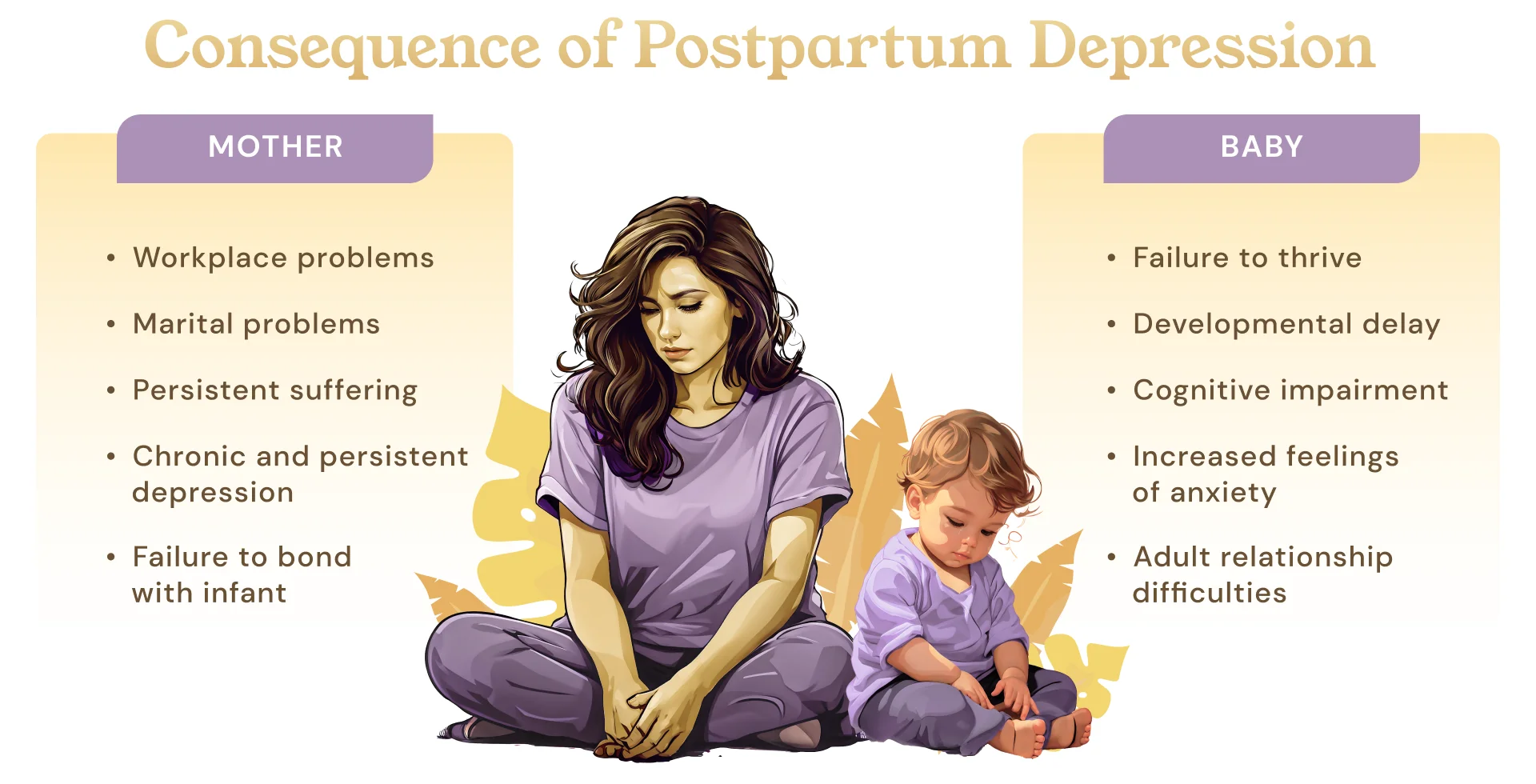
What are the consequences of untreated postpartum depression ?
Consequences to baby or infant
- Disruption to attachment and bonding between mother and baby.
- Baby can experience increase in anxiety, failure to thrive, feeding difficulty, and developmental delay.
- Infant may experience long term cognitive impairment, failure to achieve expected milestones.
- Infant may experience long term difficulty with relationships.
- Infant may experience longer-term difficulty with social or occupational functioning.

How can postpartum depression affect your marriage or relationship?
If the partner is either absent, or even if present does not understand the postpartum depression, this can cause marital or relationship difficulty, at a time when couples most need to support each other. The depressed parent may feel impatient, or angry with the partner. Likewise, the partner may feel angry and resentful due to lack of emotional and physical intimacy. Couples may stop doing the things they used to enjoy doing together such as travel, going to the gym, seeing friends, evenings out.
Untreated postpartum depression, can increase the chance of marital discord, separation, and divorce.
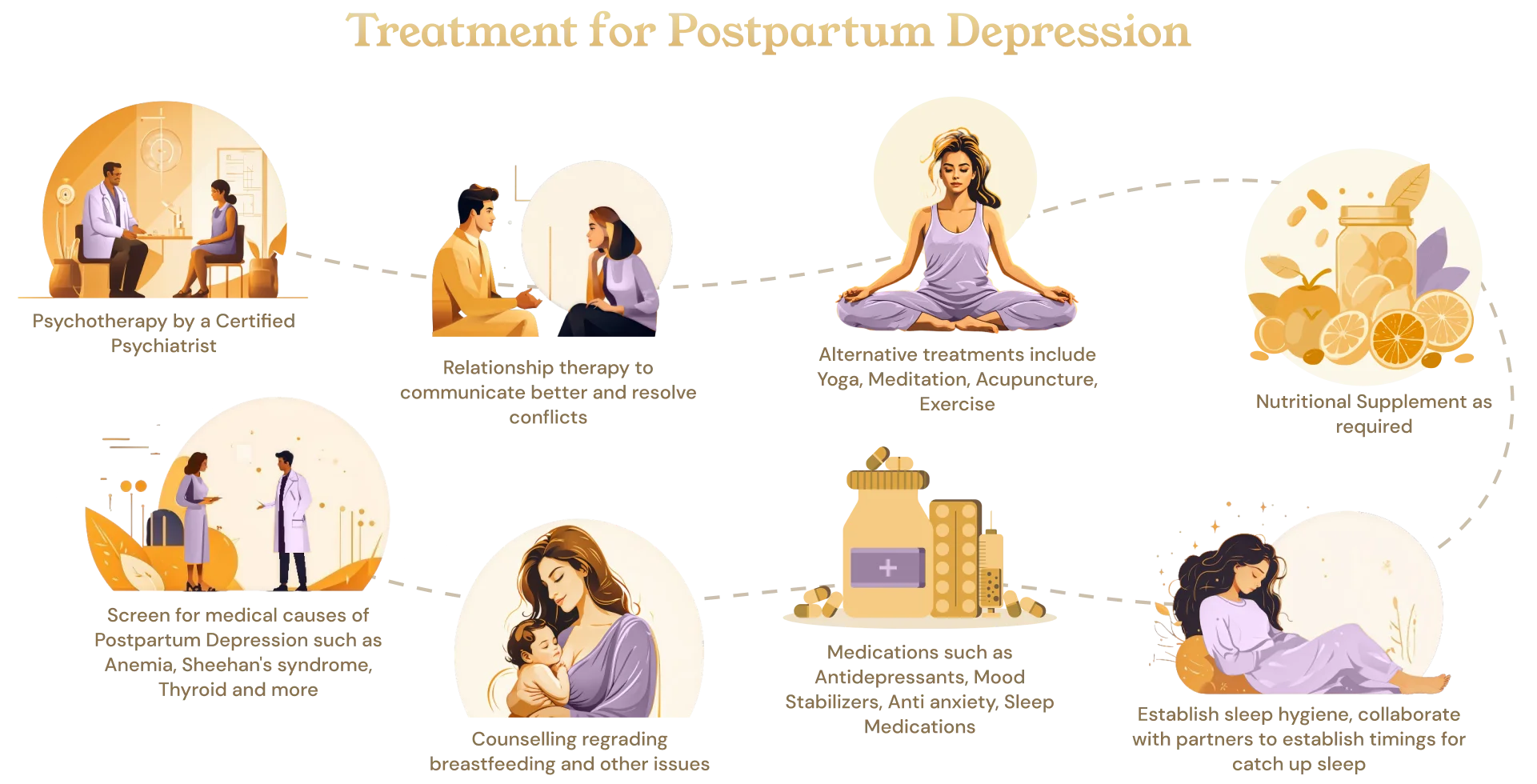
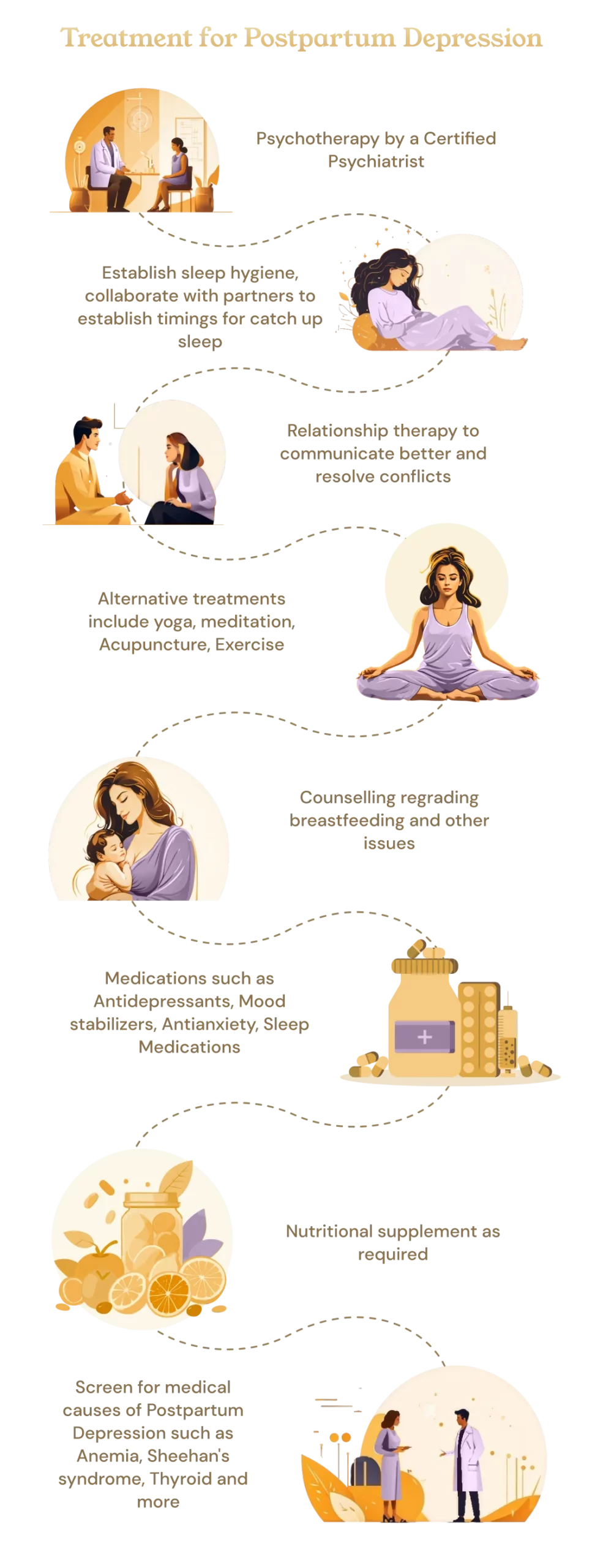
What is the treatment of postpartum depression ?
- Screen for medical causes of postpartum depression: these include anemia, thyroid disease, Sheehan’s syndrome, nutritional deficiencies, and polycystic ovarian syndrome.
- Education for both mother and partner.
- Establish sleep hygiene, and collaborate with a partner to establish times for catch-up sleep.
- Utilize resources, including childcare, and reach out to family members, including grandparents, if possible.
- Workplace documentation and accommodations. Consider what support is needed so the mother can continue working if desired or if she needs to take time off.
- Nutritional Supplementation if required.
- Counseling regarding breastfeeding and other issues.
- Psychotherapy.
- Medications if symptoms are severe.
- Alternative treatments include yoga, meditation, acupuncture, and exercise.
Should I take medication for Postpartum depression ?
It is a personal choice whether to take medication for postpartum depression. Medication is usually indicated if:
- Symptoms Postpartum depression are severe or persistent.
- Symptoms are interfering with your ability to take care of your child or children.
- Symptoms are interfering with your ability to bond with your child.
- Symptoms are interfering with your ability to take care of your family.
- Interfering with your ability to engage with your partner.
- Symptoms are negatively affecting personal or workplace relationships.
- Interfering with your ability to perform at work.
Natural treatments or alternatives have not been effective.
What medications are used to treat postpartum depression ?
It is a purely personal decision whether you choose to take medication or not. If you are choosing medications, it must be chosen carefully to ensure the least number of side effects. The medications are carefully titrated and also, should be non-addictive.
The most common worry for new mothers, breastfeeding their baby, is the exposure to the medications and it’s side-effects. Many mothers switch to half formula and half breastmilk, to minimize the chances of exposure.
Depending on your symptoms, your psychiatrist may prescribe antidepressants, mood stabilizers, antianxiety, and sleep medications. A close collaboration with your psychiatrist is essential for the best treatment plan.
Can I take antidepressants if I am breastfeeding?
Many antidepressants are classed as ‘schedule C.’, which means they are safe in pregnancy and breastfeeding. Psychiatric Medications which are considered safe in breastfeeding:
– Have been found to be safe in clinical studies.
– Are largely metabolized and are only found in breast milk in trace amounts.
Ultimately it is a personal decision, and a mother must work with her psychiatrist to evaluate the potential risks versus benefits. Depending on theseverity of symptoms and the level of impairment, a mother may decide whether to continue breastfeeding or bottle feed instead if medication is required.
Breast milk is considered to be better than formula milk as it has the correct chemical composition of nutrients and electrolytes and because it contains antibodies and bacteria virus particles in trace amounts, which stimulates the baby’s immune system. Formula milk has come a long way since ‘breast is best.’ commercials in the eighties and nineties and is much closer in chemical composition to breast milk. It is considered an acceptable alternative to bottle feeding in most cases. In the case of severe postpartum depression, the benefits of treating the mother to the baby, is considered to outweigh the loss of benefit of breastfeeding. However, formula milk does not contain hormones or maternal antibodies.
One option is a combination of breast and bottle feeding so that the baby gets some of the benefits of breast milk, including exposure to antibodies, but also has the nutritional benefit of formula milk. This combination schedule means that the baby gets the benefits of breast milk but is only exposed to a very small amount of medication, as most of its feed comes from formula milk. It is important to work closely with your doctor to formulate the best treatment plan if you are breastfeeding and plan to start medication.
Postpartum Depression and work
Mothers experiencing postpartum depression may find they are having problems with fatigue, motivation, attention, concentration, reasoning productivity, engagement with colleagues. They may find they are unable to complete tasks, meet deadlines or are taking excessive time off work. Mothers experiencing postpartum depression are more likely to be passed over for promotion, or terminated form their current position. If left untreated, mothers may find themselves falling off the career ladder, and as time passes find they are unable to get on track.
From treatment of symptoms, childcare support, communication with HR, documentation for accommodations, and leave including short term disability is required to ensure that you receive the support that you need from the workplace. Even if you decide the next best step is to take time off work, treatment is necessary to ensure that you can start a new job with a more flexible schedule, or less demanding workload when you are ready, so that you can return to your previous level of performance.


Contact Us
All you have to do is call us or schedule an appointment online via our website. Our clinical services are available in New York, South Carolina, Tennessee, Illinois, Florida, New Jersey, and California.
Gaba telepsychiatry is an online platform where the assessment can be performed via telecommunication from the client’s comfortable space.
Dr. Gundu Reddy is a board-certified psychiatrist with ten years of experience practicing forensic psychiatry and fifteen years of experience practicing clinical psychiatry.